Scurvy was known to Hippocrates, described in book two of his Prorrheticorum and in his Liber de internis affectionibus, and cited by James Lind. Symptoms of scurvy were also described by Pliny the Elder: (i) Pliny. "49". Naturalis historiae. Vol.3.; and (ii) Strabo, in Geographicorum, book 16, cited in the 1881 International Encyclopedia of Surgery.
Scurvy at sea
In the 1497 expedition of Vasco da Gama, the curative effects of citrus fruit were known. In the 1500s, Portuguese sailors put in to the island of Saint Helena to avail themselves of planted vegetable gardens and wild-growing fruit trees. Authorities occasionally recommended plant food to prevent scurvy during long sea voyages. John Woodall, the first surgeon to the British East India Company, recommended the preventive and curative use of lemon juice in his 1617 book, The Surgeon's Mate. In 1734, the Dutch writer Johann Bachstrom gave the firm opinion, "scurvy is solely owing to a total abstinence from fresh vegetable food, and greens." Scurvy had long been a principal killer of sailors during the long sea voyages. According to Jonathan Lamb, "In 1499, Vasco da Gama lost 116 of his crew of 170; In 1520, Magellan lost 208 out of 230;... all mainly to scurvy."
The first attempt to give scientific basis for the cause of this disease was by a ship's surgeon in the Royal Navy, James Lind. While at sea in May 1747, Lind provided some crew members with two oranges and one lemon per day, in addition to normal rations, while others continued on cider, vinegar, sulfuric acid or seawater, along with their normal rations, in one of the world's first controlled experiments. The results showed that citrus fruits prevented the disease. Lind published his work in 1753 in his Treatise on the Scurvy.
Fresh fruit was expensive to keep on board, whereas boiling it down to juice allowed easy storage, but destroyed the vitamin (especially if it was boiled in copper kettles). It was 1796 before the British navy adopted lemon juice as standard issue at sea. In 1845, ships in the West Indies were provided with lime juice instead, and in 1860 lime juice was used throughout the Royal Navy, giving rise to the American use of the nickname "limey" for the British. Captain James Cook had previously demonstrated the advantages of carrying "Sour krout" on board by taking his crew on a 1772–75 Pacific Ocean voyage without losing any of his men to scurvy. For his report on his methods the British Royal Society awarded him the Copley Medal in 1776.
The name antiscorbutic was used in the eighteenth and nineteenth centuries for foods known to prevent scurvy. These foods included lemons, limes, oranges, sauerkraut, cabbage, malt, and portable soup. In 1928, the Canadian Arctic anthropologist Vilhjalmur Stefansson showed that the Inuit avoided scurvy on a diet largely of raw meat. Later studies on traditional food diets of the Yukon First Nations, Dene, Inuit, and Métis of Northern Canada showed that their daily intake of vitamin C averaged between 52 and 62mg/day.
Discovery
- Further information: Vitamin §History
Vitamin C was discovered in 1912, isolated in 1928 and synthesized in 1933, making it the first vitamin to be synthesized. Shortly thereafter Tadeus Reichstein succeeded in synthesizing the vitamin in bulk by what is now called the Reichstein process. This made possible the inexpensive mass-production of vitamin C. In 1934, Hoffmann–La Roche bought the Reichstein process patent, trademarked synthetic vitamin C under the brand name Redoxon, and began to market it as a dietary supplement.
In 1907, a laboratory animal model which would help to identify the antiscorbutic factor was serendipitously discovered by the Norwegian physicians Axel Holst and Theodor Frølich, who when studying shipboard beriberi, fed guinea pigs their test diet of grains and flour and were surprised when scurvy resulted instead of beriberi. Unknown at that time, this species did not make its own vitamin C (being a caviomorph), whereas mice and rats do. In 1912, the Polish biochemist Casimir Funk developed the concept of vitamins. One of these was thought to be the anti-scorbutic factor. In 1928, this was referred to as "water-soluble C", although its chemical structure had not been determined.
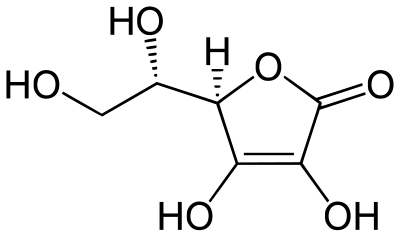
From 1928 to 1932, Albert Szent-Györgyi and Joseph L. Svirbely's Hungarian team, and Charles Glen King's American team, identified the anti-scorbutic factor. Szent-Györgyi isolated hexuronic acid from animal adrenal glands, and suspected it to be the antiscorbutic factor. In late 1931, Szent-Györgyi gave Svirbely the last of his adrenal-derived hexuronic acid with the suggestion that it might be the anti-scorbutic factor. By the spring of 1932, King's laboratory had proven this, but published the result without giving Szent-Györgyi credit for it. This led to a bitter dispute over priority. In 1933, Walter Norman Haworth chemically identified the vitamin as - l-hexuronic acid, proving this by synthesis in 1933. Haworth and Szent-Györgyi proposed that L-hexuronic acid be named a-scorbic acid, and chemically - l-ascorbic acid, in honor of its activity against scurvy. The term's etymology is from Latin, "a-" meaning away, or off from, while -scorbic is from Medieval Latin scorbuticus (pertaining to scurvy), cognate with Old Norse skyrbjugr, French scorbut, Dutch scheurbuik and Low German scharbock. Partly for this discovery, Szent-Györgyi was awarded the 1937 Nobel Prize in Medicine, and Haworth shared that year's Nobel Prize in Chemistry.
In 1957, J. J. Burns showed that some mammals are susceptible to scurvy as their liver does not produce the enzyme - l-gulonolactone oxidase, the last of the chain of four enzymes that synthesize vitamin C. American biochemist Irwin Stone was the first to exploit vitamin C for its food preservative properties. He later developed the idea that humans possess a mutated form of the - l-gulonolactone oxidase coding gene.
Stone introduced Linus Pauling to the theory that humans needed to consume vitamin C in quantities far higher than what was considered a recommended daily intake in order to optimize health.
In 2008, researchers discovered that in humans and other primates the red blood cells have evolved a mechanism to more efficiently utilize the vitamin C present in the body by recycling oxidized - l-dehydroascorbic acid (DHA) back into ascorbic acid for reuse by the body. The mechanism was not found to be present in mammals that synthesize their own vitamin C.
History of large dose therapies
- Further information: Vitamin C megadosage and Intravenous ascorbic acid
Vitamin C megadosage is a term describing the consumption or injection of vitamin C in doses comparable to or higher than the amounts produced by the livers of mammals which are able to synthesize vitamin C. An argument for this, although not the actual term, was described in 1970 in an article by Linus Pauling. Briefly, his position was that for optimal health, humans should be consuming at least 2,300mg/day to compensate for the inability to synthesize vitamin C. The recommendation also fell into the consumption range for gorillas—a non-synthesizing near-relative to humans. A second argument for high intake is that serum ascorbic acid concentrations increase as intake increases until it plateaus at about 190 to 200 micromoles per liter (μmol/L) once consumption exceeds 1,250 milligrams. As noted, government recommendations are a range of 40 to 110mg/day and normal plasma is approximately 50μmol/L, so "normal" is about 25% of what can be achieved when oral consumption is in the proposed megadose range.
Pauling popularized the concept of high dose vitamin C as prevention and treatment of the common cold in 1970. A few years later he proposed that vitamin C would prevent cardiovascular disease, and that 10 grams/day, initially administered intravenously and thereafter orally, would cure late-stage cancer. Mega-dosing with ascorbic acid has other champions, among them chemist Irwin Stone and the controversial Matthias Rath and Patrick Holford, who both have been accused of making unsubstantiated treatment claims for treating cancer and HIV infection. The idea that large amounts of intravenous ascorbic acid can improve outcomes of late-stage cancer or ameliorate the toxicity of chemotherapy is—some forty years after Pauling's seminal paper—still considered unproven and still in need of high quality research.